According to the U.S. Library of Medicine (NIH), methadone is used to relieve severe pain in people who are expected to need pain medication around the clock for a long time and who cannot be treated with other medications. It also is used to prevent withdrawal symptoms in patients who were addicted to opiate drugs and are enrolled in treatment programs in order to stop taking or continue not taking the drugs.
Methadone is in a class of medications called opiate (narcotic) analgesics. Methadone works to treat pain by changing the way the brain and nervous system respond to pain. It works to treat people who were addicted to opiate drugs by producing similar effects and preventing withdrawal symptoms in people who have stopped using these drugs.
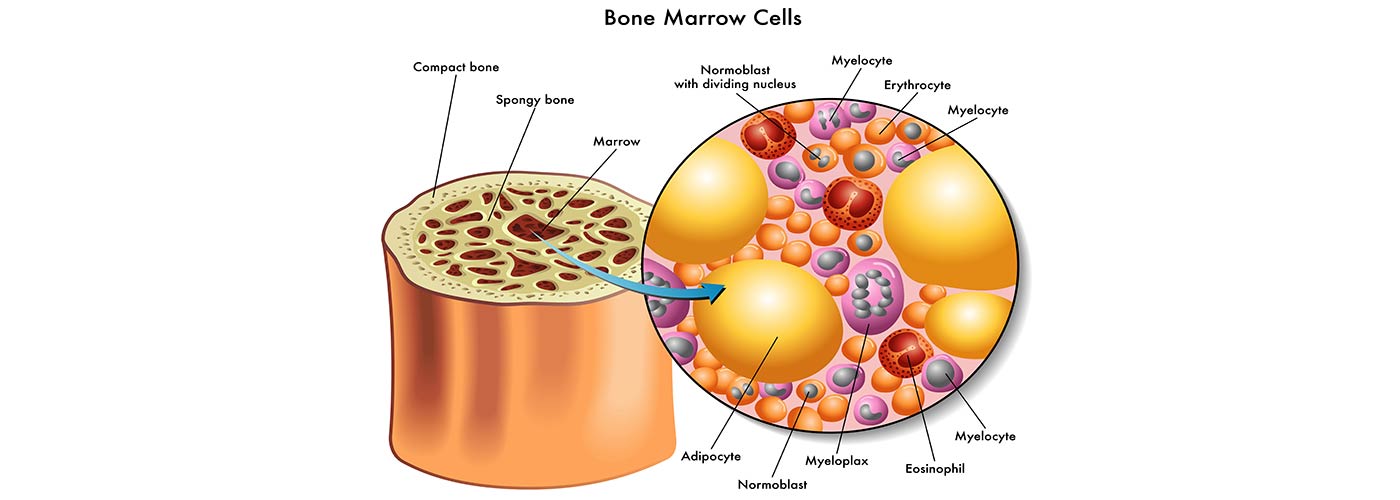
Table of Contents
How Was Methadone Created?
Methadone was created in Germany around World War II to treat pain. It didn’t make its way to the United States till after the war but was not widely used due to the painkillers misunderstood side effects it caused. Like most painkillers, patients started becoming addicted to the drug and it wasn’t until the early ‘90s that it was used regularly in the treatment of other opioid addiction called Methadone Maintenance Treatment (MMT).
3 Myths About Methadone
There are common myths about all things in life especially about the misconceptions of what a drug can or can’t do. What the side effects are and what these drugs do to persons that use them for long periods of time. Methadone has myths as well such as:
➤ Myth: Methadone damages your body.
➤ Fact: When taken properly, there is no known damage to any parts of the body. There are some side effects such as constipation, increased sweating, and dry mouth; but these go away over time or with dose adjustments.
➤ Myth: Methadone produces abnormalities in babies.
➤ Fact: Women can have a healthy pregnancy if taking the methadone as prescribed.
➤ Myth: Methadone gets into your bones and weakens them.
➤ Fact: Methadone does not “get into the bones” or cause any harm to the skeletal system. Most bone and joint aches are usually mild withdrawal symptoms.
The question of “does methadone get in your bone marrow?” has been researched and been concluded that, Yes, it does get into your bone marrow but no, like the myth was busted above, it does not weaken them.
There has been some evidence showing that methadone is present in the bone marrow of patients but if there are skeletal issues, it’s due to other factors outside of methadone maintenance. Other factors that may weaken methadone users bones and cause weakness and/or pain is:
- Lack of proper nutrition
- Pre-existing skeletal issues
- Drug/alcohol abuse
- Anemia
- Compromised immune system
How Long Has Methadone Been Around?
Methadone has been around for quite some time and for good reason because it effectively helps those dealing with chronic pain and/or drug addiction. To receive methadone maintenance treatment, you must be enrolled in a treatment program that is approved by the state and federal governments and must treat patients according to specific federal laws. Methadone must be taken under the care of professional staff unless otherwise directed.
There have been many studies about the pros and cons. It even has been included on the World Health Organization’s List of Essential Medicines for treatment for heroin dependence. Research on MMT has found some pros to be:
- MMT significantly reduces drug injecting
- Because it reduces drug injecting, MMT reduces HIV transmission
- MMT significantly reduces the death rate associated with opioid dependence
- MMT reduces criminal activity by opioid users
We are Here to Help with Methadone Addiction
We at Garden State Treatment Center understand the struggles of trying to quit methadone and can help you safely detox off it. Located in the heart of Northern New Jersey, Garden State Treatment Center is an outpatient and partial care addiction treatment facility that offers nuanced levels of care for individuals struggling with the horrors of substance abuse. It is our explicit goal to help addicted clients rebuild their lives from the inside out and reintegrate themselves back into society.
FAQ
Does Methadone get in your Bone Marrow?
Is it dangerous to take Methadone under supervised care?
Published on: 2020-03-21
Updated on: 2024-05-24



